When patients search for gum recession surgery before and after, they are usually not looking for dramatic marketing photos. They want a clear answer to a practical question: how much can the gumline actually improve, how uncomfortable is recovery, and will the result look natural months later. Those are the right questions, because the success of recession treatment is not measured by a photo taken the next day. It is measured by root coverage, tissue stability, reduced sensitivity, and a gum contour that remains healthy over time.
What gum recession surgery is meant to change
Gum recession means the gum margin has moved apically – in simple terms, it has shifted downward on lower teeth or upward on upper teeth, exposing part of the root. Patients usually notice one of three things first: the tooth looks longer, cold sensitivity increases, or the gumline becomes uneven.
Surgery is not always the first step, but when recession is significant, progressive, esthetically visible, or associated with root sensitivity, non-surgical care often has limits. A soft tissue graft or another periodontal plastic surgery technique is used to improve tissue thickness, reposition the gumline, and protect the root surface.
The “before and after” difference can be very real, but it depends on anatomy. Some cases achieve almost complete root coverage. Others improve sensitivity and tissue thickness substantially while leaving a small amount of root exposure. A responsible treatment plan starts with that distinction.
Gum recession surgery before and after: what changes visually
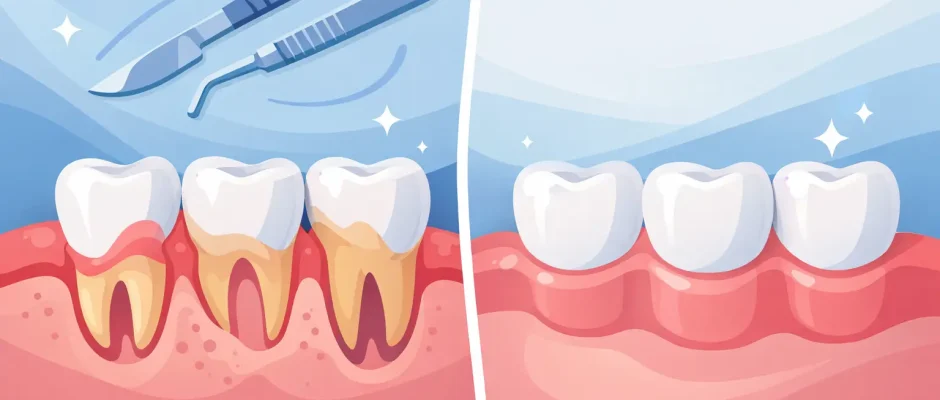
Before surgery, the affected tooth often appears longer than neighboring teeth. The exposed root may look darker or more yellow than enamel. In thin-gum patients, the tissue can appear fragile, with a narrow band of keratinized tissue and a noticeable notch-like recession defect near the neck of the tooth.
After successful surgery and healing, the gumline usually looks more symmetrical, the root is less visible or fully covered, and the tissue appears thicker and more stable. This is especially important in the smile zone, where even a 1-2 mm difference can change the overall appearance.
What patients should understand is that the immediate postoperative view is not the final result. In the first days, the area may look swollen, overbuilt, or irregular. Sutures and protective dressings can make the site appear worse before it looks better. The meaningful “after” assessment is usually done weeks to months later, not on day two.
The best-case result
In favorable cases – usually isolated recession defects with good bone support, limited inflammation, and careful oral hygiene – the final result can look remarkably natural. The gum margin blends with adjacent tissue, the color match is good, and the tooth no longer draws attention. Sensitivity often decreases significantly once the root is covered and the tissue becomes thicker.
The realistic result
Not every case ends with perfect coverage. If recession is deep, the papillae have flattened, the tooth was moved outside the bony envelope, or there is cervical wear, the improvement may be partial. Even then, surgery can still be worthwhile because increased tissue thickness and better root protection may reduce symptoms and slow future breakdown.
Why one patient’s after result looks better than another’s
This is where clinical planning matters more than internet photos. The final appearance depends on the type of recession, thickness of the soft tissue, position of the tooth, bite-related trauma, presence of non-carious cervical lesions, smoking status, and plaque control.
Technique matters as well. A coronally advanced flap, connective tissue graft, free gingival graft, tunnel technique, and use of biologic adjuncts are not interchangeable in every case. The goal is not simply to move tissue upward. The goal is to create stable, well-vascularized coverage with minimal tension.
Microsurgical principles improve precision here. Fine suturing, atraumatic tissue handling, and magnification help preserve blood supply and reduce unnecessary trauma. In practical terms, that often translates into better healing quality and a more refined esthetic outcome.
The healing timeline: what “after” actually means
Patients are often surprised by how staged the healing process is. The first week is about wound protection, not appearance. Swelling, tightness, and color changes are normal. If a graft was taken from the palate, the donor area may be more bothersome than the recipient site.
By two to three weeks, the tissue usually looks calmer, but it may still seem uneven or slightly bulky. This does not mean the result is poor. Soft tissue maturation takes time.
At around six to eight weeks, many patients begin to recognize the real contour change. The gumline looks more integrated, and the area feels less tender during brushing. Final maturation can continue for several months, especially in grafted sites.
This is one reason experienced surgeons are careful with promises. A “before and after” photo taken too early can be misleading in both directions – either unrealistically flattering or unnecessarily discouraging.
What recovery feels like
Most patients describe gum recession surgery as more manageable than they expected, especially when the procedure is done with careful local anesthesia and a structured postoperative protocol. Discomfort is usually moderate rather than severe. The bigger challenge is not pain itself but the need to protect the area from brushing trauma, chewing pressure, and lip movement during early healing.
Diet is temporarily restricted to softer foods. Oral hygiene has to be modified. Follow-up matters, because small issues such as plaque accumulation, suture irritation, or premature brushing can compromise the result.
PRF and minimally traumatic techniques may support healing in selected cases, but they do not replace fundamentals. Stable flap design, tension-free closure, and patient compliance remain the backbone of a predictable outcome.
Who is a good candidate for surgery
The strongest candidates are patients with localized recession, good general periodontal health, controlled brushing habits, and realistic expectations. Surgery is often especially helpful when recession affects visible front teeth, causes sensitivity, or progresses despite conservative measures.
A patient is not a good surgical candidate if inflammation is uncontrolled, home care is poor, or the recession is being actively driven by ongoing trauma. Aggressive brushing, clenching, an unstable bite, smoking, or orthodontic positioning outside the alveolar bone can all affect the result. In these situations, surgery without correcting the cause can lead to disappointment.
That is why consultation should include more than measuring millimeters of recession. It should evaluate the reason the recession developed in the first place.
Gum recession surgery before and after: questions to ask at consultation
A useful consultation is not centered on whether surgery can be done. It is centered on whether surgery can be done predictably in your case. Ask what percentage of root coverage is realistic, whether tissue thickness can be improved, what technique is being recommended and why, and what factors may limit the final esthetic result.
It also makes sense to ask about donor tissue versus alternative materials, healing time, brushing restrictions, and how success will be measured after surgery. If the recession is near a crown, veneer, or cervical filling, that should be discussed before the procedure because restorative contours can affect the soft tissue outcome.
For patients considering treatment in Israel, especially in a surgical practice focused on microsurgery and implantology such as Implantolog.co.il, this level of planning is not a luxury. It is what reduces uncertainty and turns a cosmetic concern into a controlled clinical procedure.
When surgery is worth it – and when it may not be
Surgery is usually worth it when recession is progressing, sensitivity is persistent, the esthetic concern is significant, or the tissue is so thin that long-term stability is questionable. It can also be worthwhile before restorative or orthodontic treatment if the soft tissue condition needs to be improved first.
It may not be worth it when the defect is very minor, symptoms are absent, and the patient is unlikely to follow postoperative instructions. It may also need to be postponed if periodontal inflammation is active or if the underlying traumatic factor has not been corrected.
The right decision is not based on fear of recession alone. It is based on whether the procedure is likely to create a stable, meaningful improvement.
Photos can be helpful, but they are only the starting point. The real value of gum recession surgery is not a dramatic before-and-after image. It is the combination of healthier tissue, less sensitivity, better long-term protection, and a result that still looks natural after healing is complete.
Comments (0)