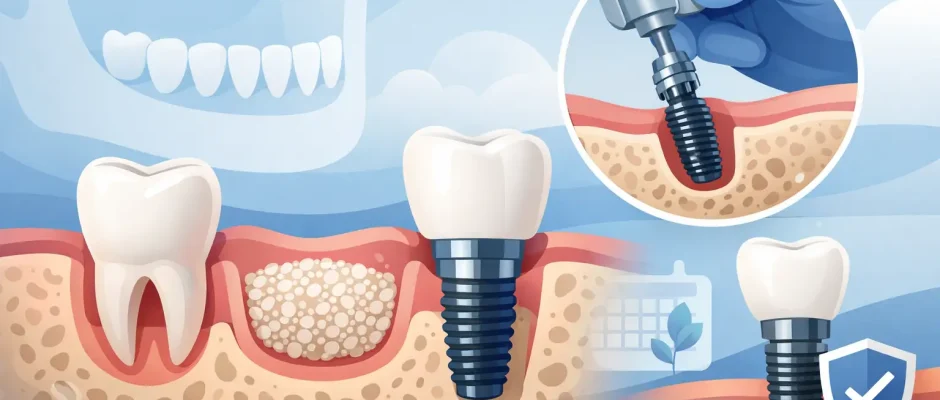
A patient often asks the same question right after hearing they need grafting: how long until the implant? That is the right question, because an implant after bone graft is not just about waiting a fixed number of months. It is about whether the new bone is stable enough, vascular enough, and shaped well enough to support a predictable result.
In practice, the timeline depends on what kind of graft was done, how much bone was missing, whether infection was present, and whether the site can achieve primary implant stability. Some patients are candidates for immediate placement. Others get a better long-term outcome by staging treatment and allowing the graft to mature first.
Implant after bone graft – what determines the timing?
There is no single healing clock for every case. A small socket preservation graft after extraction is very different from a lateral ridge augmentation or sinus lift in the posterior maxilla. The biology, the volume of grafted material, and the mechanical demands on the future implant all matter.
The most important factor is stability. An implant needs enough quality bone to lock into place at insertion. If the bone is too soft or still remodeling actively, the implant may not integrate predictably. Rushing at this stage can create a problem that is much harder to fix later.
A second factor is blood supply. Grafted bone is not instantly the same as native bone. It has to remodel, integrate, and become vascularized. This is why two sites that look similar on a scan may still behave differently clinically.
A third factor is the reason grafting was needed in the first place. If bone loss followed chronic infection, long-term tooth absence, trauma, or periodontal disease, the treatment plan has to account for that history. Good surgery starts with diagnosis, not with a generic timeline.
When can an implant be placed after a bone graft?
In straightforward cases, implant placement may be possible around 3 to 4 months after a minor graft. In more advanced cases, 4 to 6 months is common. Large augmentations may require 6 to 9 months, and occasionally longer. These are not promises. They are planning ranges.
For example, after a simple socket graft done at the time of extraction, the bone often heals enough for implant placement within a few months. After guided bone regeneration for a horizontal defect, more healing may be needed. After sinus augmentation, timing depends on residual native bone height and whether the implant was placed simultaneously or must wait.
This is where CBCT imaging becomes valuable. A 3D scan helps assess bone volume, density pattern, anatomic limitations, and the relationship to adjacent roots, the sinus, or the inferior alveolar nerve. Digital planning does not replace surgical judgment, but it makes timing and implant positioning much more precise.
Immediate implant placement and grafting at the same surgery
Sometimes the best option is not to wait at all. If a tooth is being removed and the remaining bone can provide strong primary stability, the implant may be placed immediately, with grafting used to fill residual gaps or contour the ridge.
This approach reduces overall treatment time and can help preserve soft tissue architecture. But it is not automatically the most advanced or the best option. It only works well when infection is controlled, the socket anatomy is favorable, and the implant can be stabilized in native bone.
Patients often assume immediate treatment is always preferable because it sounds faster. In reality, speed matters less than predictability. A staged approach can be the safer and more esthetic choice when bone deficiency is significant.
Delayed implant placement after graft maturation
If the defect is larger, or if the extraction site has compromised walls, placing the graft first and allowing it to heal is often the more disciplined plan. This gives the tissues time to regenerate and lets the surgeon rebuild the future implant site instead of trying to compromise within limited anatomy.
In these cases, delayed placement usually offers better control of implant position, angulation, and esthetic tissue support. That matters especially in the smile zone, where a millimeter can change the final outcome.
What affects healing before an implant after bone graft?
Healing is not determined by the graft material alone. Surgical technique, flap design, tension-free closure, membrane stability, and protection of the grafted volume are all part of the equation. Micromotion and early contamination can interfere with regeneration.
Patient factors matter too. Smoking, uncontrolled diabetes, active periodontal disease, poor oral hygiene, and heavy bite forces can all slow healing or reduce predictability. Even a technically excellent graft can fail if biology and aftercare are ignored.
The type of material used also influences the timeline. Autogenous bone, allograft, xenograft, and composite grafting each remodel differently. Faster turnover is not always better if it comes with greater volume loss. Slower-resorbing materials can help preserve contour but may require a different healing strategy.
PRF is often used as part of a biologically supportive protocol because it can improve handling of graft materials and support soft tissue healing. It is not magic, and it does not replace sound surgical principles, but in the right setting it can be a useful adjunct.
How your surgeon decides the site is ready
The decision is not based on the calendar alone. The site is evaluated clinically and radiographically. The soft tissue should be healthy, without ongoing inflammation or dehiscence. The grafted ridge should have adequate width and height for prosthetically correct implant placement, not just enough bone to fit a fixture somewhere.
A CBCT may show whether the planned implant can be placed in an ideal position with safe distances from neighboring structures. In many cases, guided planning and surgical templates improve accuracy, especially when the available bone is limited or the esthetic demands are high.
During surgery, tactile feedback still matters. Bone can look promising on imaging but feel immature at osteotomy preparation. Experienced implant surgery is partly digital and partly biological judgment in real time.
Risks of placing the implant too early
The main risk is poor osseointegration. If the implant does not achieve adequate stability or the grafted site has not matured enough, integration may be incomplete or fail altogether. That can mean additional surgery, more healing time, and greater expense.
There is also a prosthetic risk. If the implant is forced into a compromised position because the ridge is not fully reconstructed, the final crown may be less esthetic, harder to clean, or biomechanically overloaded. A successfully integrated implant is not the same thing as a well-restored implant.
Early placement can also increase the chance of soft tissue recession in visible areas. For front teeth, this is one of the biggest reasons treatment planning must be conservative when the anatomy is borderline.
What patients can do during healing
The most useful step is to protect the surgical site and follow the post-op plan exactly. That includes medication use as prescribed, oral hygiene adjustments, dietary restrictions, and avoiding pressure from removable appliances unless they have been specifically adjusted for the graft.
Smoking cessation is one of the most meaningful ways to improve healing. If gum inflammation or untreated periodontal disease is present elsewhere in the mouth, it should be controlled before implant placement. Long-term success depends on the whole mouth, not only the grafted area.
Patients should also understand that healing milestones can change after follow-up visits. If the site needs more time, that is not bad news. It usually means the plan is being adapted to biology instead of forcing biology to match a schedule.
A more predictable way to think about timing
The better question is not, how fast can I get the implant? It is, when will the site be ready for an implant that has the best chance to last. That mindset changes everything.
For some patients, an implant after bone graft can be placed quite soon. For others, waiting protects the final result. The right answer comes from imaging, examination, surgical history, and a treatment plan built around stability and long-term function.
If you are considering treatment and want a plan based on anatomy rather than guesswork, that is exactly where careful digital diagnostics and microsurgical protocol make a difference. At https://implantolog.co.il, the goal is not simply to place an implant, but to place it at the right time, in the right position, with the highest level of predictability.
A few extra months of disciplined healing can save years of compromise later.
Comments (0)