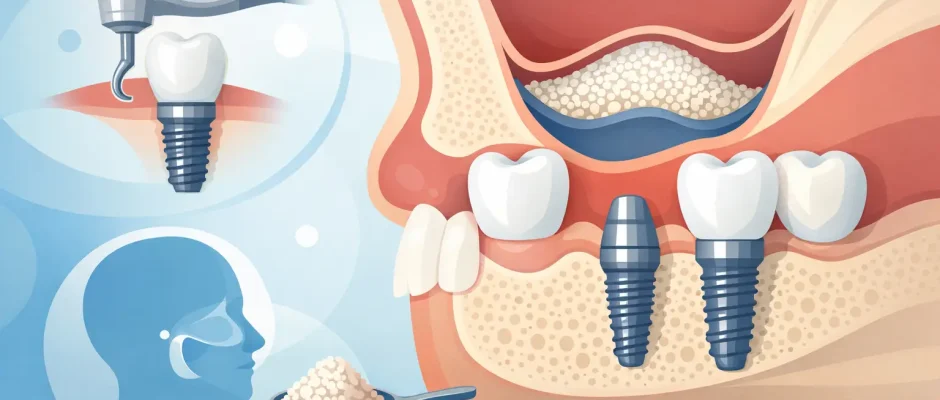
Losing an upper back tooth often creates a second problem that patients do not expect – not just the missing tooth, but too little bone to place an implant safely. In this area, the maxillary sinus sits directly above the roots of the premolars and molars. After extraction, bone can shrink while the sinus gradually expands downward. That is the situation where a sinus lift becomes relevant.
For many patients, the phrase sounds intimidating. In practice, sinus lift surgery for implants is a well-established bone augmentation procedure used to create enough vertical bone in the upper jaw for stable implant placement. The goal is straightforward: build the foundation first, then place the implant in a position that is safe, functional, and long-lasting.
What sinus lift surgery for implants actually does
A sinus lift, also called sinus augmentation, increases bone height in the posterior upper jaw. During the procedure, the sinus membrane is gently elevated, and bone graft material is placed beneath it. Over time, this area matures into new bone that can support a dental implant.
This matters because implants depend on primary stability and long-term bone support. If the remaining bone is too thin or too short, forcing an implant into that site creates unnecessary risk. The implant may have poor initial stability, be placed in a compromised angle, or fail under load later. In other words, skipping bone preparation to save time can cost more treatment time in the future.
Not every upper jaw implant requires a sinus lift. If enough native bone remains, an implant can often be placed without grafting. But when the sinus is low and the bone height is limited, augmentation may be the difference between a predictable result and a compromise.
When a sinus lift is recommended before implants
The decision is based on anatomy, not preference. A clinical exam and CBCT scan show the available bone height and width, the shape of the sinus floor, the presence of sinus septa, and the condition of the sinus membrane.
A sinus lift is commonly recommended when a patient has lost upper molars or premolars long ago, when bone resorption has progressed after extraction, or when the sinus has pneumatized into the space where the tooth roots used to be. It can also be part of treatment in complex rehabilitation cases where implant positioning must be prosthetically driven rather than simply placed wherever bone happens to remain.
There are also situations where a sinus lift is not the right first step. Active sinus disease, unresolved periodontal infection, smoking-related healing concerns, or uncontrolled systemic conditions may require correction before surgery. Good planning means knowing not only how to perform augmentation, but when to postpone it.
Types of sinus lift surgery for implants
There are two main approaches, and the right one depends mostly on how much bone is already present.
Internal sinus lift
An internal, or crestal, sinus lift is performed through the implant site itself. It is generally used when a moderate amount of native bone remains and only limited vertical gain is needed. In selected cases, implant placement can be done at the same appointment.
This approach is less invasive, but it is not automatically better. Its indication is narrower, and success depends on proper case selection, careful membrane handling, and accurate implant planning.
Lateral window sinus lift
A lateral sinus lift is used when bone deficiency is more pronounced. A small access window is created in the side wall of the upper jaw, the membrane is elevated under direct vision, and graft material is placed into the new space.
This technique offers excellent control in advanced defects and is often the preferred option when substantial bone gain is needed. Depending on residual bone height and implant stability, implants may be placed simultaneously or after a healing period.
What happens during the procedure
For most patients, the surgery is more controlled than they imagine. Local anesthesia is usually sufficient, and the area is carefully prepared to minimize trauma. If a lateral approach is used, the bony window is opened, the Schneiderian membrane is gently detached and elevated, and graft material is inserted into the created space. The site is then closed with fine sutures.
In modern surgical practice, precision makes a significant difference. Digital planning helps define implant position before the first incision. In selected cases, surgical guides support accurate placement. Atraumatic technique, good soft tissue handling, and biologic support methods such as PRF can improve healing conditions and reduce postoperative discomfort.
The procedure itself usually does not feel painful because of anesthesia. What patients notice more often is pressure, vibration, and the unfamiliar idea of surgery near the sinus. This is where clear communication matters. When each step is explained in advance, anxiety usually drops significantly.
Can implants be placed at the same time?
Sometimes yes, sometimes no. This depends on the amount and quality of the remaining native bone and whether it can provide adequate primary stability for the implant.
If residual bone is sufficient, simultaneous implant placement can shorten treatment time and avoid an additional surgery. If bone is very limited, a staged approach is safer. First the sinus is augmented, then the graft is allowed to mature, and only after that are implants placed.
Patients often prefer the faster option, which is understandable. But the faster option is not always the more predictable one. In implant surgery, stability and correct positioning matter more than compressing the timeline.
Recovery and what to expect after surgery
Most patients experience swelling, mild to moderate soreness, and a feeling of pressure in the upper jaw or cheek area for several days. Bruising is possible. These reactions are expected and usually manageable with prescribed medications and routine postoperative care.
For a short period after surgery, patients are asked to avoid blowing the nose, sneezing with the mouth closed, heavy lifting, forceful rinsing, and other actions that sharply increase sinus pressure. These instructions are not minor details. They directly protect the surgical site and help prevent membrane disruption.
Healing is not only about how you feel in the first week. Bone maturation takes longer. Depending on the graft volume, anatomy, and treatment plan, healing before implant loading may take several months. This can feel slow, but biologic stability is what supports a long-term result.
Risks, complications, and how they are managed
A sinus lift is predictable when planned properly, but it is still surgery. The most common intraoperative complication is perforation of the sinus membrane. Small perforations can often be repaired during the procedure. Larger ones may require a change in the plan.
Other possible issues include infection, graft loss, sinusitis, bleeding, delayed healing, or insufficient bone formation. Smoking, poor compliance with instructions, and untreated dental or sinus pathology can raise these risks.
This is one reason surgeon experience matters in advanced implant cases. Managing anatomy, recognizing limitations, and adjusting the protocol when conditions change are part of the treatment, not separate from it. The patient sees a single procedure. The surgeon sees tissue behavior, membrane quality, implant biomechanics, and long-term restorative goals all at once.
Why planning matters more than the graft material alone
Patients often ask which graft material is best. That question makes sense, but it is only one part of the result. The more important issue is whether the treatment plan matches the anatomy and the prosthetic objective.
A well-executed sinus lift starts with diagnosis. CBCT analysis, evaluation of the sinus cavity, assessment of residual bone, and understanding the future restoration all shape the protocol. The implant should not just fit into available bone. It should emerge in the right position for function, hygiene, and esthetics.
That is why advanced implant care increasingly relies on digital planning, microsurgical technique, and structured protocols rather than improvised decisions during surgery. On https://implantolog.co.il, this approach is central: reduce uncertainty before treatment, perform surgery with precision, and make each step understandable for the patient.
Is a sinus lift worth it?
If the upper jaw lacks bone, the real comparison is not between a sinus lift and a simple implant. The real comparison is between creating proper support and accepting a compromised foundation.
For many patients, sinus augmentation makes it possible to place implants where they otherwise would not be possible, or to place them in a position that gives a better long-term restorative result. It adds time and complexity, but in the right case it also adds safety and predictability.
The best next step is not to assume you need it, or to hope you can avoid it. It is to get a proper examination and a CBCT-based treatment plan. When the anatomy is clear, the path forward usually becomes clear as well – and that tends to replace fear with something much more useful: confidence.
Comments (0)