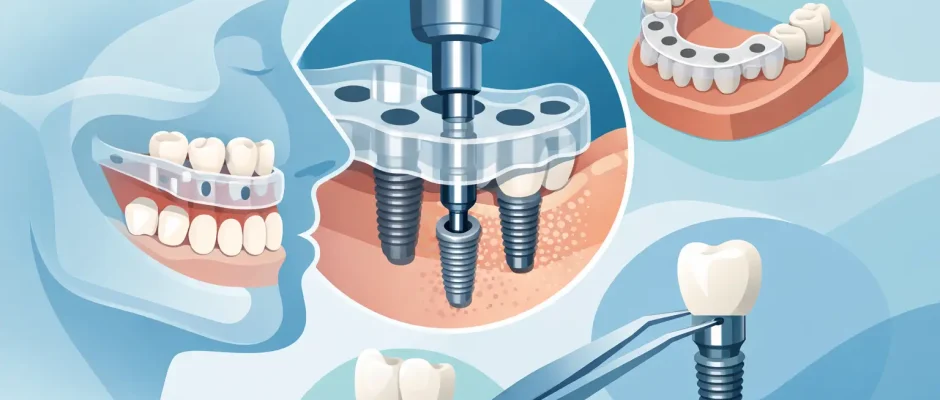
When a patient says, “I want the implant placed exactly where it should be,” they are describing the reason guided surgery exists.
A surgical guide for dental implants is not a marketing extra and not a decorative plastic template. It is a clinical tool created from digital planning data to transfer the planned implant position into the mouth with a high level of precision. For many patients, that means a safer procedure, more predictable prosthetic positioning, and often a more comfortable surgical experience.
At the same time, not every case should be treated the same way. Guided implant surgery is powerful, but like any protocol in surgery, it works best when it is selected for the right indication and executed with discipline.
What is a surgical guide for dental implants?
A surgical guide for dental implants is a custom-made template used during implant placement. It is designed after digital diagnostics, usually based on a CBCT scan and an intraoral scan or other accurate model of the teeth and soft tissues. The guide helps the surgeon place the implant at the planned angle, depth, and position.
In practical terms, this matters because an implant is not just a titanium screw placed into bone. Its position affects the future crown, the contour of the gum, cleaning access, load distribution, and the relationship to nearby anatomical structures such as the maxillary sinus, adjacent roots, or the inferior alveolar nerve.
That is why experienced implant surgeons plan from the final result backward. The ideal restoration guides the implant position, not the other way around.
How guided implant surgery works
The process starts with diagnostics. A clinical examination is combined with imaging and an assessment of bone volume, soft tissue condition, bite, and esthetic demands. If the case is suitable, implant planning software is used to choose implant diameter, length, angulation, and exact restorative position.
After that, the guide is fabricated, typically with digital manufacturing methods. During surgery, the guide is seated on the teeth, mucosa, or bone depending on the clinical situation. Special sleeves or guided instrumentation help the surgeon prepare the osteotomy according to the digital plan.
This is where patients often feel reassured: the operation is not based on estimation during the procedure. It is based on a preoperative plan that has already considered the anatomy and the prosthetic goal.
Still, a guide does not replace surgical judgment. It transfers a plan. The quality of that plan, the stability of the guide, and the surgeon’s ability to verify every step remain essential.
Why a surgical guide for dental implants can improve outcomes
The main advantage is predictability. In implantology, a few degrees of angulation or a small positional error can change the prosthetic result significantly. A guided approach reduces that risk, especially in areas where space is limited or esthetics are demanding.
For a single front tooth, precision is critical because even a small deviation can affect the emergence profile and soft tissue symmetry. In posterior areas, the guide may help avoid anatomical structures and improve load distribution. In full-arch concepts such as All-on-4, accurate planning becomes even more important because multiple implants must work together prosthetically.
There is also a comfort factor. In selected cases, guided surgery may allow for a less invasive approach with a smaller flap or flapless placement. That can reduce postoperative swelling and make recovery easier. But this depends on bone anatomy, keratinized tissue, visibility, and the need for additional procedures such as bone grafting.
This is a good example of where “less invasive” is not always automatically “better.” If visibility is compromised or bone augmentation is required, opening the area properly may be the safer and more responsible option.
When guided surgery is especially useful
A surgical guide is particularly valuable in cases where margin for error is small. That includes implants near the sinus or mandibular nerve, narrow interdental spaces, high-esthetic-zone restorations, and full-arch rehabilitation.
It is also useful when immediate implant placement is planned after extraction. In these cases, the anatomy can be deceptive because the extraction socket does not always guide the implant toward the ideal restorative position. The guide helps the surgeon avoid following the socket in the wrong direction and instead place the implant where the final tooth needs it to be.
Patients with bone deficiency can also benefit from detailed digital planning. If bone volume is limited, the implant trajectory must often be optimized carefully. Sometimes that makes guided placement more valuable. In other cases, the anatomy is so compromised that grafting and conventional intraoperative decision-making become more important than a strict fully guided protocol.
Are there limitations?
Yes, and this deserves an honest answer.
A surgical guide for dental implants is only as accurate as the data and protocol behind it. If the scan quality is poor, the digital merge is inaccurate, or the guide does not seat perfectly, precision can be affected. Even small errors in each step can accumulate.
There are also practical limitations. In patients with limited mouth opening, placing guided instruments in posterior regions may be difficult. In cases with mobile soft tissue support, a mucosa-borne guide can be less stable than a tooth-supported one. During immediate placement after extraction, the guide helps, but the surgeon still must manage primary stability and the three-dimensional anatomy of the socket carefully.
This is why guided surgery should not be presented as autopilot. It is a tool inside a surgical system, not a substitute for training and experience.
Does guided implant surgery mean no flap and no pain?
Not necessarily.
Patients often associate guided surgery with flapless implant placement, minimal trauma, and very easy healing. Sometimes that is true. If bone volume is adequate, soft tissue conditions are favorable, and the implant position is straightforward, a flapless guided approach can be an excellent option.
But many real clinical cases are more complex. If the surgeon needs to assess bone directly, contour the ridge, perform guided bone regeneration, use PRF, or improve soft tissue management, opening a flap may still be indicated. That does not mean the treatment is less advanced. It means the protocol is being adapted to biology rather than forced into a simplified workflow.
For patient comfort, anesthesia, gentle tissue handling, precise planning, and careful postoperative follow-up usually matter more than whether the procedure is marketed as flapless.
What patients should ask before choosing this option
A patient does not need to understand planning software in detail, but they should understand the logic of the treatment. Ask whether the implant is being planned from the future crown position, whether a CBCT is part of the diagnostic protocol, and whether the guide is being used because it improves the case – not just because it sounds modern.
It is also reasonable to ask what happens if the intraoperative situation differs from the plan. A competent implant surgeon should be comfortable with both digital planning and real surgical adaptation. Predictability comes from preparation, but safety also depends on judgment during the operation.
If your case involves extraction, bone loss, sinus lift, or immediate loading, the discussion should be even more specific. The right question is not “Do you use guides?” The better question is “Why is this protocol appropriate for my anatomy and my final restorative goal?”
The real value of a guided approach
The best use of a surgical guide is not simply to place an implant faster. Its real value is to make treatment more controlled.
Controlled treatment tends to be safer. It is usually easier to explain to the patient. It supports more predictable restorative work. And in many cases, it reduces the number of intraoperative surprises, which is exactly what most patients want before surgery.
On the other hand, serious implantology is never about one tool. A good result depends on diagnostics, three-dimensional planning, atraumatic technique, primary stability, soft tissue management, bone biology, and follow-up. A guide improves one critical part of that chain.
For patients considering treatment, this is often the most reassuring perspective: digital protocols are useful not because they look advanced, but because they help the surgeon work with greater precision and fewer compromises. That is the standard many patients are looking for when they choose implant treatment in the first place.
If you are evaluating implant therapy, look for a plan that is calm, specific, and anatomically sound. Technology should make the treatment clearer and safer for you – not more confusing.
Comments (0)