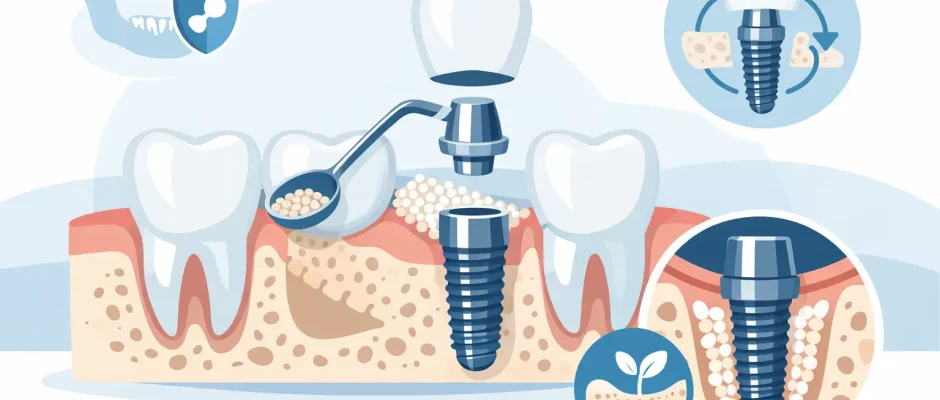
A patient usually hears the same unsettling phrase at the implant consultation: “There may not be enough bone.” That is exactly where a clear guide to implant placement with bone deficiency becomes useful – not to oversimplify the problem, but to explain what the lack of bone really means, when it changes the plan, and when it does not.
Bone deficiency is common. It develops after tooth loss, chronic infection, trauma, long-term denture use, periodontal disease, or natural sinus anatomy in the upper jaw. The key point is this: reduced bone volume does not automatically mean implants are impossible. It means the case requires more careful diagnostics, better planning, and the right surgical protocol.
What bone deficiency actually changes
An implant needs stable surrounding bone in order to integrate and carry chewing forces predictably. When bone height or width is reduced, the surgeon has fewer safe and reliable options for positioning the implant in the ideal restorative position. That affects more than just whether an implant can be placed. It also affects implant diameter and length, primary stability, esthetics, long-term load distribution, and proximity to important structures such as the maxillary sinus or the inferior alveolar nerve.
This is why experienced implant planning starts with 3D imaging rather than guesswork. A CBCT scan shows not only how much bone is present, but where it is missing, how dense it is, and whether the defect is localized or generalized. In many cases, the decision is not “implant or no implant.” The real decision is which sequence gives the safest and most predictable result: immediate placement, simultaneous grafting, staged bone augmentation, sinus floor elevation, or an alternative restorative strategy.
Guide to implant placement with bone deficiency: first decisions
The first part of any guide to implant placement with bone deficiency is understanding timing. Some cases can be treated in one surgical stage, while others benefit from staged treatment. Neither approach is automatically better. It depends on anatomy, infection control, soft tissue condition, and the ability to achieve primary implant stability.
If a tooth is being removed and the remaining socket walls are largely intact, immediate implant placement may still be possible even when bone volume is not ideal. In that setting, the implant is anchored in the available native bone, and the residual gap may be managed with grafting material and a membrane. This can shorten treatment and help preserve tissue architecture.
If bone loss is more advanced, trying to place an implant too early can compromise positioning or stability. In those cases, a staged protocol is usually the more responsible choice. First, the site is reconstructed with guided bone regeneration or another augmentation technique. After healing and maturation, the implant is placed into a better foundation. This takes longer, but longer is not the same as worse. In many advanced defects, it is the more predictable path.
Horizontal vs vertical bone loss
Not all defects behave the same way. Horizontal loss means the ridge becomes too narrow. Vertical loss means the ridge is too short in height. Horizontal augmentation is generally more straightforward and more predictable than vertical augmentation. Vertical reconstruction can be highly effective in selected cases, but it is more technique-sensitive and places greater demands on healing and soft tissue management.
This distinction matters because patients often ask, “Can you just add bone?” Sometimes yes, but the complexity varies considerably depending on the defect geometry.
Bone grafting is not one procedure
Bone grafting is often discussed as if it were a single treatment. It is not. Guided bone regeneration may involve particulate graft material, autogenous bone chips, collagen or non-resorbable membranes, fixation, and meticulous soft tissue closure. In the posterior upper jaw, the main issue may be reduced vertical height due to sinus expansion, and the solution may be a sinus lift rather than ridge augmentation alone.
The surgical goal is not to “fill a space.” The goal is to create a biologically stable environment in which new bone can form and mature around the future or newly placed implant. That is why technique matters. A graft that looks acceptable on the day of surgery can still fail if the flap design is poor, if the membrane becomes exposed, if the site is overloaded, or if the patient smokes heavily and healing is impaired.
PRF can also be useful as part of a biologically supportive protocol. It is not a magic shortcut, but in the right clinical context it may support soft tissue healing and improve handling of the grafted site.
When a sinus lift becomes part of the plan
In the upper back jaw, bone deficiency often has less to do with disease and more to do with anatomy after tooth loss. As the sinus expands and the ridge resorbs, the available bone height under the sinus floor decreases. This is one of the most common reasons a sinus lift is recommended.
A crestal sinus lift may be sufficient when a moderate amount of height is missing and implant stability can still be achieved. A lateral window sinus augmentation is more often chosen when the deficit is greater. Again, the decision is based on measurements, residual bone height, sinus anatomy, membrane condition, and prosthetic goals.
Patients sometimes worry that a sinus lift makes treatment unusually risky. In experienced hands, it is a routine part of advanced implant surgery. That said, it remains a real surgical procedure and should be planned with the same discipline as any other augmentation technique.
Digital planning matters more in difficult cases
When bone is limited, freehand surgery leaves less room for error. Digital planning and surgical guides become especially valuable because they help align the implant position with both the available anatomy and the future prosthetic restoration.
This is not just a technology story. It is a safety story. In a narrow ridge or near critical anatomical structures, a few millimeters matter. A guided approach can reduce positional compromise, improve restorative outcomes, and support more conservative use of the remaining bone.
For complex cases, the best result comes from planning backward from the final tooth position and then selecting the surgical method that makes that position achievable. That is far more reliable than placing an implant where bone happens to exist and trying to adapt the crown later.
What patients should realistically expect
A practical guide to implant placement with bone deficiency should also address expectations. Advanced implant cases usually require more than one appointment, more healing time, and closer follow-up. The trade-off is a more stable long-term foundation.
Discomfort is usually manageable and often less severe than patients expect, especially when microsurgical principles, careful tissue handling, and clear postoperative instructions are part of the protocol. Swelling and temporary functional limitations are normal after augmentation procedures. What matters is that the patient understands the sequence in advance.
The timeline may range from immediate implant placement with simultaneous grafting to several months of staged healing before the implant is placed and later restored. Faster treatment is appealing, but speed should never override biological predictability.
Not every patient needs the same solution
Two patients can both be told they have “bone loss” and still need completely different treatment. One may be a good candidate for immediate placement with contour grafting. Another may need extraction, healing, ridge reconstruction, and delayed implant placement. A third may be better served by a full-arch concept such as All-on-4, where implant positioning relies on the remaining strategic bone rather than rebuilding every lost area.
That is why generic promises are not useful in this field. The right plan is individualized.
Questions worth asking at the consultation
If you are considering implants in a site with reduced bone volume, ask how the bone deficiency was measured, whether the implant can be placed in the ideal restorative position, whether grafting is simultaneous or staged, and what the surgeon sees as the main risk in your specific case. These questions usually tell you more than marketing claims.
It is also reasonable to ask what is included in the surgical plan: imaging, anesthesia, membrane use, PRF, guided surgery, follow-up visits, and the expected healing intervals. Clarity reduces anxiety because it replaces vague promises with a defined protocol.
In advanced implantology, confidence should come from planning, not from optimism alone. A careful surgeon does not minimize complexity, but also does not dramatize it. Bone deficiency is a challenge, not a verdict. With the right diagnostics, disciplined technique, and a treatment plan built around your anatomy rather than a one-size-fits-all template, implant rehabilitation can remain both safe and highly predictable. If your case is complex, that usually means you need more precision – not less hope.
Comments (0)