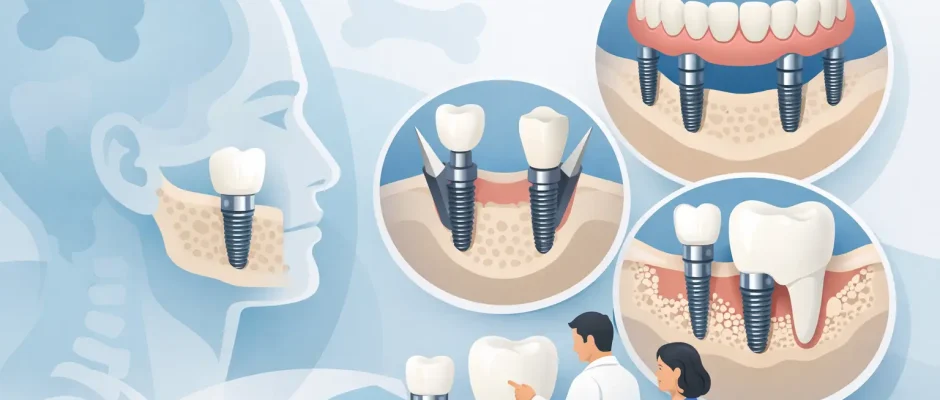
If you were told that there is “not enough bone for implants,” that is not a diagnosis of failure. It is a planning problem. And in many cases, the best implant options for bone atrophy are not about finding one magical technique, but choosing the right protocol for your anatomy, bite, sinus position, gum condition, and long-term goals.
This is where patients often get conflicting opinions. One doctor recommends bone grafting. Another suggests short implants. A third proposes an angled full-arch solution. All of these can be correct in the right case. The key question is not which method sounds easier, but which one gives the most predictable and stable result with the lowest surgical burden for that specific patient.
What bone atrophy really changes
Bone loss after tooth extraction is not just a matter of volume on a scan. The jaw changes in width, height, and density. In the upper jaw, the sinus may expand downward, leaving very little vertical bone. In the lower jaw, the nerve canal limits how deep an implant can be placed. In long-standing tooth loss, the gum and soft tissue often become thinner as well, which affects esthetics and hygiene.
That is why implant planning in atrophic bone is a surgical and prosthetic decision at the same time. The implant must integrate into bone, but it also needs to emerge in a position where the final crown or bridge will function well and be easy to clean. A solution that avoids grafting but forces a compromised prosthetic angle is not always the best solution.
Best implant options for bone atrophy: it depends on the defect
There is no universal “best” option. The best approach depends on whether the bone deficiency is mild, moderate, or severe, whether one tooth or a full arch is missing, and whether immediate loading is realistic.
For mild to moderate horizontal bone loss, guided bone regeneration is often one of the most rational choices. In practical terms, this means rebuilding the missing width of the ridge with bone graft material and a membrane, sometimes combined with PRF to support healing. This approach is especially useful when the implant position is otherwise ideal but the ridge is too thin for safe placement. It preserves prosthetic logic instead of forcing the surgeon to place the implant where bone happens to remain.
For vertical loss in the posterior upper jaw, a sinus lift may be the most predictable option. If residual bone height is sufficient, implant placement and sinus augmentation can sometimes be performed in one stage. If the bone is very limited, a staged approach is safer. Patients usually prefer a faster path, but a slower protocol can be the more responsible one when primary stability is questionable.
Short implants are another important option and, in the right case, they are not a compromise. Modern short and ultra-short implants can perform well when bone width is adequate, occlusal load is controlled, and the prosthetic design is favorable. They can reduce surgical trauma and avoid sinus lift or vertical augmentation in selected patients. But they are not a shortcut for every case. If a patient has heavy bite forces, parafunction, poor crown-to-implant ratio, or insufficient ridge width, short implants may not be the best long-term bet.
Angled implants and full-arch concepts such as All-on-4 can be excellent solutions when multiple teeth are missing and posterior bone is deficient. By using available anterior bone and tilting distal implants, it is often possible to avoid more invasive grafting procedures. This can shorten treatment time and make fixed teeth possible even in advanced atrophy. At the same time, this concept has to be executed with careful digital planning and precise surgical positioning. Small errors in angulation or implant distribution can create major prosthetic problems later.
When bone grafting is worth it
Patients often ask whether bone grafting can be skipped. Sometimes yes. Sometimes skipping it creates a result that is faster now and more fragile later.
Bone grafting is usually worth serious consideration when the missing bone would force poor implant positioning, when esthetics matter in the smile zone, or when long-term tissue stability is part of the treatment goal. In the front of the mouth, this matters especially. Even if an implant can technically be inserted into a narrow or deficient ridge, the final result may show gum recession, gray shine-through, or an unnatural contour.
In these cases, augmentation is not an “extra” procedure. It is part of building a result that looks and functions like a tooth replacement rather than a mechanical fixture in bone.
The trade-off is time and healing. Bone regeneration and staged implant placement often require patience. But in complex anatomy, patience is part of risk control.
Guided bone regeneration
Guided bone regeneration is commonly used when the ridge is too thin. It can be done at the time of implant placement if sufficient primary stability is achievable, or before implant placement if the defect is larger. The advantage is better implant positioning and improved support of the surrounding tissues. The limitation is healing time and the fact that outcomes depend heavily on surgical technique, flap management, and postoperative control.
Sinus augmentation
A sinus lift is relevant when upper back teeth have been missing for a long time and the sinus has expanded. This is a very common reason patients hear that there is “not enough bone.” In experienced hands, sinus augmentation is a routine and predictable procedure, but it still requires proper indication, careful membrane handling, and realistic timing.
When shorter or alternative implants make more sense
Not every patient benefits from grafting. Some want to reduce the number of surgeries. Others have medical factors, smoking history, or healing concerns that make a less invasive path more sensible.
Short implants are often attractive in the posterior jaws where esthetics are less critical and anatomical limits are clear. They can reduce treatment time and discomfort. Zygomatic implants exist for extreme upper jaw atrophy, but they are a highly specialized solution reserved for advanced cases, not a routine first-line option.
For full-arch rehabilitation, tilted implants may allow fixed teeth without extensive grafting. This is often valuable for patients who have worn dentures for years and want a stable restoration with fewer stages. Still, the surgical convenience should never overshadow prosthetic planning. A full-arch case succeeds when implant positions support a durable bridge, balanced load distribution, and hygiene access.
How digital planning improves safety in atrophic bone
In difficult bone anatomy, planning from a simple two-dimensional X-ray is not enough. CBCT-based planning shows the actual available bone, the sinus, the nerve, the ridge angulation, and the restorative space. That information changes decisions.
A surgical guide can further improve accuracy, especially when implants must be placed in a narrow anatomical corridor or according to a full-arch prosthetic plan. This does not replace surgical judgment. It supports it. In complex cases, digital planning and guided surgery help reduce guesswork and improve reproducibility.
Micro-surgical technique matters too. Gentle tissue handling, primary closure when needed, stable graft protection, and biologic support such as PRF can make healing calmer and more predictable. Patients usually experience this not as a technical detail, but as less swelling, less anxiety, and a smoother recovery.
How to choose between the best options
The best implant options for bone atrophy are usually chosen after answering four practical questions. How much bone is missing, and in which direction? Is this a single tooth, several teeth, or a full arch? Is the patient prioritizing the shortest path, the least invasive surgery, the best esthetic outcome, or the most conservative long-term architecture? And finally, what level of surgical complexity is justified by the expected benefit?
A good treatment plan explains not only what can be done, but what is being traded. A grafted solution may offer better implant positioning and tissue stability, but takes longer. A short-implant solution may reduce surgery, but not in every bite situation. A full-arch tilted concept may avoid major augmentation, but requires excellent execution and maintenance.
That is why second opinions differ. The anatomy may allow several valid paths. What matters is whether the recommendation is built around predictability rather than convenience.
If you are evaluating implants after being told you have bone loss, ask for a plan that starts with imaging, explains the defect clearly, and compares at least two realistic treatment options. The right answer is rarely the most aggressive or the fastest one. It is the one that fits your anatomy, your goals, and your tolerance for risk with the greatest respect for long-term stability.
Comments (0)