A missing tooth changes more than your smile. Within weeks after extraction, the bone in that area begins to shrink, neighboring teeth can start to shift, and chewing load is redistributed in ways that are not always obvious at first. That is why patients asking about best ways to replace a tooth after extraction are usually not looking for a cosmetic fix alone. They want a solution that is stable, safe, and predictable.
The right option depends on four things: where the tooth was removed, how much bone remains, the condition of the adjacent teeth, and how quickly you want to restore function and appearance. In surgical dentistry, there is rarely one universal answer. There is, however, a clear logic for choosing well.
Best Ways to Replace a Tooth After Extraction: What Actually Works
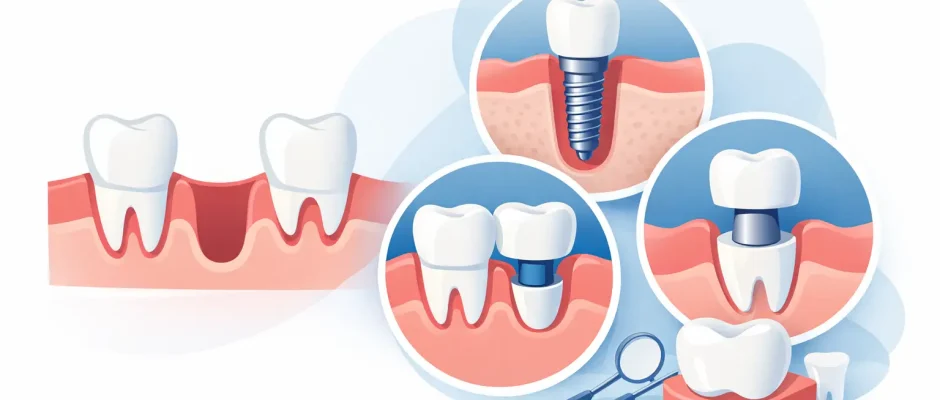
In modern practice, there are three main ways to replace a missing tooth: a dental implant, a fixed bridge, or a removable prosthetic solution. They are not equal in long-term biology, comfort, or preservation of surrounding tissues.
A dental implant is usually the most physiologic option when conditions allow. It replaces the root as well as the crown, which helps preserve chewing function and reduces overload on neighboring teeth. It also avoids grinding down healthy adjacent teeth, which is often necessary for a traditional bridge.
A fixed bridge can still be a reasonable treatment in selected cases, especially if the teeth next to the gap already have large fillings or crowns and need restoration anyway. The trade-off is that a bridge relies on those teeth for support. If they are healthy and untouched, sacrificing tooth structure may not be the best long-term decision.
A removable option is typically the least desirable for a single missing tooth, but it may be used as a temporary solution or when surgery is contraindicated. It is usually less comfortable, less stable during chewing, and does not prevent bone loss in the extraction site.
Why implants are often the first-choice solution
When patients ask for the best replacement rather than the cheapest or fastest one, implants are often at the center of the conversation. The reason is straightforward: they restore the missing tooth without recruiting neighboring teeth into the treatment plan.
From a functional standpoint, an implant helps reestablish chewing efficiency in a more natural way. From a structural standpoint, it transmits load to the bone, which matters because the jawbone needs stimulation to maintain volume. No restoration can stop all remodeling after extraction, but an implant generally supports better long-term tissue stability than leaving the site empty or using a removable appliance.
Esthetics also matter, especially in the smile zone. A well-planned implant restoration can support natural gum contours, but this is where timing and technique become critical. If the tooth has already been missing for a long time, or if infection, trauma, or thin bone are involved, additional procedures may be needed to create a stable foundation.
This is why implant treatment should not be reduced to the question, “Can an implant be placed?” The better question is, “Can it be placed in the right position, with enough hard and soft tissue support, for a predictable long-term result?”
Immediate implant after extraction vs delayed implant
Patients are often told that an implant can be placed right after tooth removal. In some cases, that is true and highly effective. Immediate implantation can shorten treatment time and help preserve tissue architecture. It is especially attractive when the tooth is in the front and maintaining gum shape is important.
But immediate placement is not automatically the best choice. It depends on the integrity of the socket walls, the presence or absence of acute infection, soft tissue quality, bite forces, and the ability to achieve strong primary stability. If those conditions are not present, rushing the timeline can compromise the outcome.
A delayed implant, placed after a period of healing, may actually be safer and more predictable in a compromised site. That is not a step backward. It is proper surgical judgment.
When bone preservation changes the future options
One of the most common mistakes after extraction is focusing only on removing the tooth and not on preserving the site. Bone resorption starts early. In some areas, especially the upper front jaw, even small volume loss can affect both esthetics and implant positioning.
Socket preservation, often using grafting materials and sometimes biologic support such as PRF, is designed to reduce post-extraction collapse. It does not freeze the bone in time, but it can significantly improve the site for future implant placement. For patients who are not ready to place an implant immediately, preserving the socket is often the move that keeps the better options open.
If bone loss is already present, treatment may still be possible with guided bone regeneration, sinus augmentation in the upper posterior jaw, or staged reconstruction. These are not exotic procedures. In experienced hands, they are standard parts of advanced implant planning.
The role of digital planning and surgical precision
The difference between an implant that simply integrates and one that is positioned for long-term success is often planning. Digital imaging allows the surgeon to assess bone dimensions, anatomy, and restorative space before treatment begins. Surgical guides can further improve precision when the case requires exact angulation and depth control.
This matters because implant dentistry is not only about placing titanium into bone. It is about placing it where the future crown, the bite, and the surrounding tissues will function together. Precision at the surgical stage reduces the need for compromise later.
When a bridge may still be the right answer
Implants are not the answer to every case. If adjacent teeth already need crowns, a bridge may be clinically reasonable and economically practical. It can also be useful when the patient prefers to avoid surgery, has medical factors that complicate implant treatment, or needs a faster path in a very specific scenario.
The key is honest case selection. A bridge can restore appearance and function well, but it does not preserve the bone at the missing tooth site. It also places load on neighboring teeth, which may be acceptable or may create future maintenance issues depending on their condition.
For some patients, especially those with advanced wear or existing restorations, that trade-off is acceptable. For others, it is not.
What about doing nothing for a while?
Some patients plan to “wait a few months” before deciding. That is understandable, especially after a difficult extraction. But waiting without a site preservation strategy can make the future treatment more complex.
The tooth next to the space may tip. The opposing tooth may over-erupt. Bone and gum volume may shrink. None of this happens dramatically overnight, but the biology does not pause just because the treatment decision does.
Sometimes a short delay is perfectly reasonable. The important part is that the delay should be managed, not accidental. A clear plan for healing, temporary restoration, and reevaluation can prevent the kind of tissue loss that limits your choices later.
How to choose the best option for your case
If you are weighing the best ways to replace a tooth after extraction, the best decision usually comes from a consultation that looks beyond the missing tooth itself. The surgeon should evaluate the extraction site, adjacent teeth, bite, smile line, tissue thickness, bone volume, and your medical history. A good plan also considers your priorities: esthetics, treatment time, budget, surgical comfort, and long-term maintenance.
In higher-demand cases, especially front teeth, thin gums, long-standing missing teeth, or bone deficiency, the value of a surgeon with implant and reconstructive experience becomes even more relevant. The treatment may involve immediate implantation, staged grafting, soft tissue management, or a temporary restoration protocol designed to protect the final result.
For patients considering treatment in Israel, especially in a surgical practice focused on implantology, this kind of structured planning can make the difference between a quick replacement and a predictable reconstruction.
The best tooth replacement after extraction is not the one that sounds most advanced. It is the one that respects your anatomy, protects future stability, and is executed with enough precision that you do not have to revisit the same problem a few years later.
Comments (0)