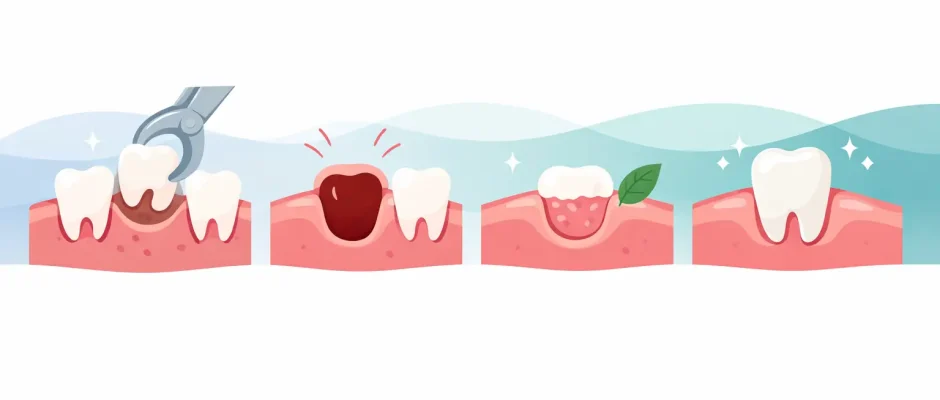
The first 24 hours after an extraction matter more than most patients expect. In that short window, your body is not just “recovering” – it is building the foundation for proper healing. Understanding tooth extraction healing stages helps you tell the difference between normal postoperative symptoms and signs that need a call to your surgeon.
Healing is not identical for every patient. A simple extraction of a mobile tooth usually recovers faster than removal of an impacted wisdom tooth, a fractured molar, or a tooth removed in preparation for implant treatment. Technique also matters. A careful surgical approach, gentle tissue handling, thorough socket management, and in some cases the use of PRF can improve comfort and support more predictable healing.
Tooth extraction healing stages: what happens first
Immediately after the tooth is removed, the socket fills with blood. That blood clot is not an incidental byproduct of surgery. It is the biological dressing that protects bone and nerve endings while signaling the body to start repair. During the first several hours, the clot stabilizes and early inflammatory cells move into the area.
At this stage, mild bleeding or blood-tinged saliva can be normal. So can numbness from local anesthesia, a dull ache once the anesthetic wears off, and gradual swelling. What should not happen is heavy active bleeding that soaks gauze continuously, severe increasing pain within the first day despite medication, or repeated forceful rinsing that dislodges the clot.
The main priority on day 1 is protection of the socket. Suction, spitting, smoking, vigorous rinsing, and strenuous exercise all increase the risk of disturbing the clot. When that clot is lost too early, healing becomes slower and more painful.
Days 2-3: inflammation peaks
For many patients, the second and third days are the least comfortable. Swelling often reaches its maximum in this period, especially after surgical extraction, wisdom tooth removal, or procedures that require flap elevation and bone contouring. Limited mouth opening can also appear, particularly in the lower jaw.
This phase can feel discouraging, but it is often normal. Inflammation is part of repair. Your immune system is cleaning the site and preparing it for the next stage. The key question is whether symptoms are following an expected pattern. Moderate swelling, tenderness, and bruising can be acceptable. Fever, foul taste, worsening asymmetrical swelling, or pain that intensifies rather than stabilizes deserve attention.
Soft food, good hydration, prescribed medication, and gentle hygiene around the area are usually enough to get through this phase. The goal is not to “speed up” biology but to avoid setbacks.
The first week of tooth extraction healing stages
By days 4-7, most uncomplicated cases begin to turn the corner. Pain usually becomes easier to manage, swelling starts to decline, and the socket develops a visible layer of healing tissue. If sutures were placed, they may still be present depending on the material used.
Inside the socket, granulation tissue forms. This is soft, vascular repair tissue that gradually replaces the blood clot. Patients sometimes worry when they see white or yellowish material in the extraction area. In many cases, that appearance is fibrin, a normal component of healing, not infection. It should not be aggressively cleaned out.
At the same time, the gum margins begin moving inward. The site still looks like a hole because bone healing always lags behind soft tissue healing. That difference is important. A socket can look improved from the outside while deeper remodeling is still in its early stages.
When dry socket tends to appear
One complication patients often hear about is dry socket, or alveolar osteitis. This usually develops between days 2 and 5 if the blood clot breaks down or is lost. The classic pattern is pain that becomes stronger instead of better, often radiating to the ear or jaw, with an unpleasant taste or odor.
Dry socket is painful, but it is not the same as infection. It is a local healing disturbance. It is more common after lower wisdom tooth extraction, smoking, traumatic surgery, previous dry socket, and sometimes oral contraceptive use. The good news is that it can be treated, and the pain usually improves significantly once the socket is professionally managed.
Weeks 2-4: soft tissue closes, bone keeps working
By the second week, the gum tissue has usually closed substantially in simple cases. If non-resorbable sutures were placed, they are often removed around this time. Chewing becomes easier, though the area may still feel tender under pressure.
This is often the stage where patients think healing is finished. Clinically, it is not. Soft tissue may look nearly normal, but the socket is still being rebuilt from the inside. Fibrous tissue is gradually replaced by immature bone, and the ridge continues to remodel.
That remodeling can be straightforward, or it can be significant if the extraction was complex or the surrounding bone was already thin. This matters when future implant placement is planned. In some cases, preserving the socket at the time of extraction helps limit volume loss and creates a more favorable foundation for prosthetic treatment.
What is normal in this phase
A mild indentation in the gum can still be present. Food may collect in the area, especially after molar extraction. Sensitivity when chewing on that side is also common. These are not necessarily signs of a problem.
What does require reassessment is persistent swelling, drainage, increasing bad taste, fever, or numbness that does not gradually improve. After lower surgical extractions, especially impacted wisdom teeth, temporary nerve irritation can occur. Most cases improve with time, but the timeline depends on the degree of nerve involvement.
One to three months: bone remodeling and functional recovery
The deeper phase of healing takes much longer than patients can see in the mirror. Over several weeks to months, the extraction socket fills with new bone and the shape of the alveolar ridge changes. This is the period that determines long-term anatomy.
If no replacement is planned, the site generally becomes asymptomatic and stable. If an implant is planned, the timing depends on the original infection, remaining bone, extraction difficulty, and whether grafting or immediate implantation was performed. There is no single correct timeline for every case. Sometimes immediate implant placement is ideal. Sometimes waiting creates a safer and more predictable result.
This is where treatment planning matters more than speed. Preserving bone and soft tissue is often more valuable than rushing to the next procedure.
What affects healing time and comfort
Not all extractions heal the same way because not all extraction sites start the same way. A tooth with active infection, a broken root, dense surrounding bone, or extensive inflammation before surgery usually heals differently than a loose periodontally compromised tooth.
Patient factors matter too. Smoking, diabetes, poor oral hygiene, immune compromise, uncontrolled periodontal disease, bruxism, and certain medications can all influence recovery. Age also plays a role, though it is rarely the only factor.
Surgical technique is another major variable. Atraumatic extraction, careful flap design, socket debridement, irrigation, stable suturing when needed, and biologically guided protocols can reduce postoperative morbidity. In a surgical practice focused on implantology and oral surgery, these details are not cosmetic. They are part of achieving a predictable healing environment.
How to support normal healing
Recovery instructions are simple, but they are not optional. Pressure on gauze, cold compresses in the first day, appropriate pain control, and temporary food modification all help. So does avoiding smoking and nicotine in any form, because reduced blood supply directly interferes with repair.
Oral hygiene should continue, just with restraint around the surgical site. Patients who stop brushing entirely often create a second problem with plaque accumulation and gum inflammation. Gentle cleaning of the rest of the mouth is beneficial, and postoperative rinses should be used exactly as directed.
If bone grafting, PRF, membrane placement, or immediate implant placement was performed, the aftercare may be more specific. That is one reason personalized instructions matter more than generic internet advice.
When to contact your surgeon
The safest rule is simple: improving symptoms usually mean normal healing, while worsening symptoms need review. Pain that suddenly intensifies after initial improvement, swelling that expands after day 3, pus, fever, persistent bleeding, difficulty swallowing, or prolonged numbness should not be ignored.
Follow-up is especially important after difficult extractions, retained roots, impacted teeth, or cases tied to future implant treatment. A good postoperative review is not a formality. It is part of making sure the socket is healing in a way that supports the next stage of care.
Healing after extraction is not a single event. It is a sequence, and each stage has its own logic. When patients know what is expected, recovery feels less alarming and far more manageable – which is often the first step toward a calmer surgical experience.
Comments (0)