Losing most or all teeth changes more than your smile. It affects chewing, speech, facial support, and often confidence in everyday situations. When patients start comparing the best full mouth implant options, they usually discover that there is no single universal answer. The right solution depends on bone volume, bite forces, medical history, esthetic demands, and how much surgery you are willing to accept.
This is where a careful treatment plan matters more than marketing terms. “Teeth in a day” may be possible for some patients, while others will get a better long-term result from a staged approach with bone augmentation and delayed loading. A predictable outcome starts with diagnosis, not with choosing a branded concept first.
What full mouth implant treatment actually means
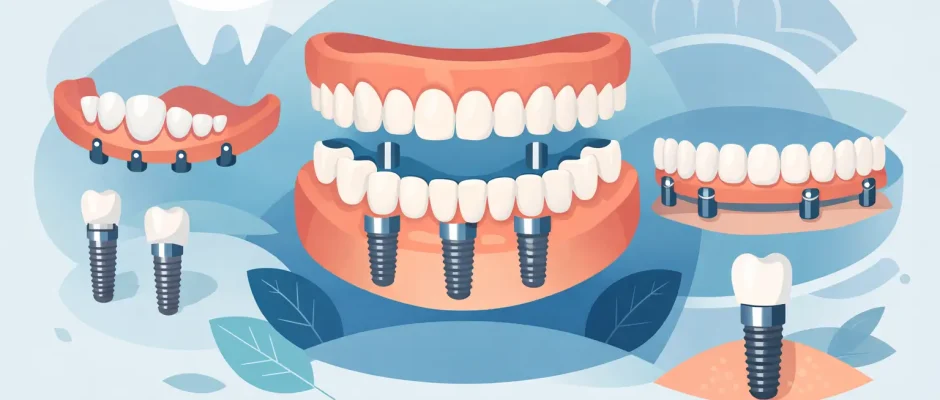
Full mouth implant rehabilitation means replacing all teeth in the upper jaw, lower jaw, or both using implants as anchors for fixed or removable prosthetics. In practice, this usually falls into three broad categories: a removable implant overdenture, a fixed full-arch bridge on a limited number of implants, or a more segmented reconstruction using a higher number of implants.
The difference is not just comfort. Each option changes how forces are distributed, how easy cleaning will be, how natural the prosthetic can look, and what happens if one implant fails. Patients often focus on the number of implants, but the real clinical question is how the entire system will function over time.
Best full mouth implant options for different clinical situations
Implant overdenture
An implant overdenture is a removable denture that snaps onto implants. It is often supported by two to four implants in the lower jaw and sometimes more in the upper jaw, where bone quality is usually softer. This option is not the most luxurious, but it can be very effective.
For patients whose current denture is loose and painful, an overdenture may feel like a dramatic improvement. Stability becomes better, chewing improves, and the prosthesis is easier to clean because it can be removed. Surgery is usually less extensive and the cost is lower than with a fixed full-arch bridge.
The trade-off is that it still remains a removable solution. Some patients never fully adapt to taking teeth out at night, and esthetics can be less refined than in a fixed reconstruction. Still, for older patients, for patients with limited bone, or for those who want to reduce surgical burden, it can be a very rational choice.
Fixed full-arch bridge on 4 to 6 implants
This is the option many patients mean when they ask about full mouth implants. A full set of fixed teeth is supported by four, five, or six implants, depending on anatomy and load distribution. All-on-4 is the best-known concept, but it is only one protocol within a larger category of full-arch treatment.
Its main advantage is that the teeth stay in place. Patients do not remove them, chewing feels more natural, and many people regain confidence quickly. In selected cases, immediate loading is possible, meaning a temporary fixed bridge can be delivered soon after surgery.
But this approach is not automatically ideal for everyone. Four implants may be sufficient in some arches, especially when posterior implants are tilted to avoid anatomical structures and increase support. In other cases, six implants provide a safer biomechanical plan, especially in patients with strong bite forces, parafunction, or larger arches. Upper jaws often need more support than lower jaws.
A fixed full-arch bridge also requires disciplined hygiene. Food retention, prosthetic screw maintenance, and regular professional follow-up are part of treatment, not an afterthought. If a patient wants fixed teeth but struggles with cleaning access, that has to be addressed before treatment begins.
More implants with segmented or individual restorations
In some patients, the best full mouth implant options are not based on the fewest implants possible. A reconstruction using more implants and segmented bridges, or even individual crowns in selected areas, can offer advantages in esthetics, load distribution, and maintenance.
This type of treatment is often considered when bone volume allows ideal implant positioning or when the patient wants a result that more closely mimics natural tooth emergence. It may also be useful in younger patients who need a long-term plan with better retrievability and easier repair of smaller sections.
The disadvantages are straightforward: more implants, more surgery, more cost, and sometimes a longer timeline. It is a more demanding path, but for the right patient it can be the most conservative prosthetic solution in the long run because it avoids overloading a minimal number of implants.
How bone loss changes the decision
Bone volume is one of the main factors that separates a simple full-arch case from a complex one. When teeth have been missing for years, the jaw often shrinks in width and height. In the upper jaw, the maxillary sinus can further reduce available bone. In these cases, the cheapest or fastest protocol may not be the safest.
Sometimes angled implants and a graft-free full-arch concept can avoid more invasive augmentation. Sometimes that is a smart decision. Sometimes it creates prosthetic compromises, poor implant angulation, or esthetic limitations that become obvious later.
In other patients, bone grafting, sinus lift surgery, or guided bone regeneration creates a better foundation for implant placement. This usually means a longer treatment course, but also a more favorable implant position and a more stable prosthetic design. The point is not that grafting is always necessary. The point is that avoiding it at any cost is not always in the patient’s best interest.
Immediate teeth vs staged treatment
One of the most common questions is whether teeth can be placed right away. The answer is yes, sometimes. Immediate implant placement and immediate provisionalization can work very well when there is enough primary stability, infection is controlled, and bite forces can be managed.
However, immediate loading should not be treated like a sales feature. If implants are placed into compromised bone, if extraction sites are infected, or if the patient has a high-risk bite pattern, a staged protocol may be more predictable. That usually means healing first, then prosthetic loading later.
A responsible surgeon does not promise speed at the expense of stability. Digital planning, surgical guides, and precise prosthetic coordination can make immediate protocols safer, but they do not cancel biology.
Materials matter, but design matters more
Patients often ask whether zirconia is better than acrylic or whether titanium is better than another implant surface. These are valid questions, but the prosthetic design, passive fit, and maintenance plan usually matter more than the material alone.
Acrylic hybrid prostheses can be lighter, more repairable, and useful as long-term temporaries or definitive solutions in selected cases. Zirconia can provide excellent esthetics and wear resistance, but it is less forgiving in some mechanical situations and requires careful planning of bite and framework support.
The same applies to implant systems. A reputable system with good evidence is important, but success depends just as much on case selection, surgical execution, tissue management, and follow-up care.
What to ask before choosing among the best full mouth implant options
Before agreeing to treatment, a patient should understand what problem the proposed plan is solving. Is the goal maximum stability with minimal surgery? Better esthetics in the smile zone? Avoiding grafts? Reducing treatment time? Preserving options if maintenance is needed later?
It is reasonable to ask how many implants are planned and why, whether bone grafting is recommended or being avoided, whether the restoration will be removable or fixed, and what happens if one implant fails. You should also know what is included in the surgical phase, the temporary phase, and the final prosthetic phase.
A clear plan lowers anxiety because it replaces vague promises with defined steps. In complex surgery, predictability is not about sounding confident. It is about showing how the decision was made.
A practical way to think about your choice
If your priority is lower cost and easier hygiene, an overdenture may be the best fit. If your priority is fixed teeth with a shorter treatment path, a full-arch bridge on four to six implants may be appropriate. If your priority is a more individualized reconstruction with fewer prosthetic compromises, a plan with more implants may be worth considering.
None of these options is automatically the “best” in isolation. The best option is the one that matches your anatomy, functional demands, and tolerance for surgery while preserving safety and long-term maintainability. In full-mouth rehabilitation, good decisions come from careful diagnostics, digital planning, and a surgical team willing to explain trade-offs clearly.
If you are comparing treatment plans, look for the one that feels medically reasoned, not just attractive on paper. The right full-mouth solution should let you eat, speak, and smile with less worry – and with a result that still makes sense years from now.
Comments (0)