Losing most or all teeth in one jaw changes more than appearance. Chewing becomes limited, speech may shift, removable dentures can feel unstable, and many patients start avoiding certain foods or social situations. That is usually the moment the question comes up: what are all-on-4 dental implants, and are they actually a reliable alternative to a full denture?
In practical terms, All-on-4 is a full-arch implant treatment. Instead of placing an implant for every missing tooth, the dentist uses four implants to support a fixed bridge for the entire upper or lower jaw. The concept is designed to restore function with fewer implants, often with a shorter and more efficient surgical plan than older full-mouth approaches.
What are all-on-4 dental implants and how do they work?
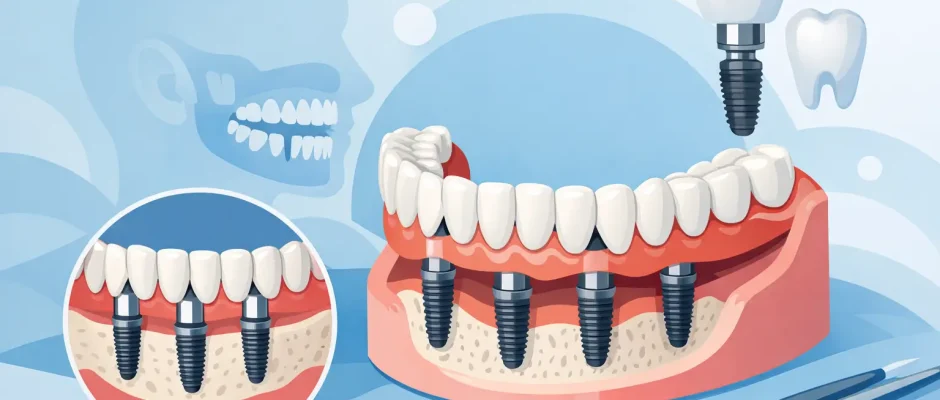
All-on-4 dental implants are a method of replacing all teeth in one arch with a fixed prosthesis supported by four strategically placed implants. Two implants are usually placed in the front part of the jaw, where bone is often denser and more stable. The two posterior implants are commonly tilted to use available bone more effectively and avoid important anatomical structures such as the maxillary sinus in the upper jaw or the nerve canal in the lower jaw.
That angulation is not a shortcut. It is a biomechanical solution. By tilting the back implants, the surgeon can often achieve better implant length and stability without moving directly into areas where bone grafting would otherwise be required.
A fixed provisional bridge may sometimes be attached soon after surgery if the implants achieve sufficient primary stability. This is why patients often hear the phrase teeth in a day. The phrase is attractive, but the real issue is not speed alone. The key question is whether the bone quality, bite, general health, and surgical stability make immediate loading safe and predictable.
Why patients choose All-on-4
For the right patient, the appeal is obvious. All-on-4 can provide fixed teeth with fewer implants, fewer surgical stages, and in some cases less need for extensive bone grafting. Compared with a removable denture, a fixed bridge usually feels more secure and functional. Patients often report better chewing efficiency, greater confidence in speaking, and a stronger sense that their teeth are part of them rather than a prosthesis they have to manage.
There is also a treatment planning advantage. In cases with failing teeth, advanced wear, severe periodontal disease, or long-standing edentulism, a full-arch solution may be more predictable than trying to save or replace teeth one by one. A fragmented approach can sometimes lead to repeated procedures, changing costs, and a compromised final bite.
That said, fewer implants does not mean simple treatment. Full-arch implant rehabilitation requires careful diagnosis, prosthetic planning, and precise surgical execution. Digital planning, CBCT imaging, and in selected cases guided surgery help reduce guesswork and improve positioning.
Who is a good candidate?
The best candidates are patients who are missing all teeth in one jaw, are close to losing the remaining teeth, or already wear dentures and want a fixed alternative. Many are dealing with loose dentures, advanced gum disease, broken teeth, or severe bone loss that makes conventional approaches more difficult.
A good candidate also needs realistic expectations. All-on-4 is not the same as getting a new set of natural teeth back. It is a highly effective prosthetic reconstruction, but it still depends on anatomy, hygiene, bite force, smoking status, and maintenance over time.
Bone volume matters, but not in a simplistic way. Some patients with reduced bone can still be treated successfully because implant angulation and careful planning make use of the remaining anatomy. Others may still need grafting, extra implants, or a different concept such as All-on-6. The phrase all-on-4 sounds standardized, but every jaw is different.
Patients with uncontrolled diabetes, active periodontal infection, severe bruxism, or heavy smoking may still be treatable, but risk assessment becomes more important. In those cases, the goal is not to sell a protocol. The goal is to choose the version of treatment with the highest chance of long-term success.
What the treatment process usually looks like
The process starts with consultation and diagnosis. This includes a clinical exam, 3D imaging, discussion of symptoms and goals, and evaluation of the remaining teeth, bone, bite, and smile line. The prosthetic outcome should be planned before surgery, not improvised after it.
If teeth need to be removed, extractions may be combined with implant placement in the same appointment when conditions allow. In the right case, this reduces the number of surgeries and shortens overall treatment time. In other cases, staged treatment is safer. This depends on infection, bone defects, soft tissue condition, and the expected ability to stabilize the implants immediately.
Once the implants are placed, a temporary fixed bridge may be delivered if the insertion torque and overall stability are adequate. If not, a different healing plan is chosen. This is one of the most important moments where experienced judgment matters. Immediate loading can be excellent when indications are right, but forcing it in a marginal case can increase complications.
After healing and osseointegration, the final prosthesis is made. This is not just a nicer-looking version of the temporary bridge. The definitive restoration is designed for long-term strength, esthetics, hygiene access, and balanced bite distribution.
Advantages of All-on-4, and where the limits are
The advantages are real. Treatment can often be faster than traditional full-arch rehabilitation, and many patients avoid wearing a removable denture during healing. Because the posterior implants are tilted, some cases can be managed without sinus lift or extensive grafting. Cost may also be lower than placing six to eight implants per arch.
But the limits matter just as much. With only four implants supporting a full arch, implant position and load distribution are critical. If one implant fails, the whole restoration may be affected. Hygiene under the bridge is also more demanding than many patients expect. Food can collect underneath, and daily cleaning with special aids is not optional.
There are esthetic limitations too. In patients with high smile lines, severe tissue loss, or asymmetry of the jaws, the transition between prosthesis and gum can become visible. That does not automatically exclude treatment, but it changes the planning. Sometimes a different prosthetic design gives a more natural result.
Is All-on-4 better than dentures or individual implants?
Compared with removable dentures, All-on-4 is usually more stable, more comfortable, and more efficient for chewing. Most patients feel a major improvement in confidence and quality of life. Still, it requires surgery, financial investment, and long-term maintenance.
Compared with placing a larger number of individual implants, All-on-4 is often more efficient and less invasive. But it is not always better. A patient with favorable bone anatomy may benefit from additional implants for improved support and prosthetic flexibility. In another case, preserving several healthy teeth and avoiding full-arch extraction may be the wiser choice.
This is where personalized planning matters. The right treatment is the one that fits the condition of the jaw, not the one with the strongest marketing name.
What affects long-term success?
Long-term success depends on three things working together: precise surgery, a well-designed prosthesis, and patient compliance. If one of these fails, the result becomes less predictable.
From the surgical side, implant positioning is everything. The implants must be placed where bone is stable and where the final bridge can function correctly. Digital planning and surgical guides can improve precision, especially in full-arch cases where small positional errors matter.
From the prosthetic side, the bridge must distribute forces properly and allow hygiene access. From the patient side, regular maintenance visits, home care, and control of risk factors such as smoking and clenching make a substantial difference.
This is also why full-arch implant treatment should not be viewed as a one-day product. Even when teeth are delivered quickly, success is built over months and then maintained over years.
The question behind the question
When patients ask what are all-on-4 dental implants, they are rarely asking for a textbook definition. What they usually want to know is whether they can eat normally again, whether the surgery will be manageable, and whether the result will feel secure rather than temporary.
A well-executed All-on-4 treatment can answer those concerns very well. But the treatment is only as good as the diagnosis, the plan, and the discipline behind every step. In complex cases, especially where bone is limited or previous dental work has failed, careful surgical judgment matters more than the label of the procedure itself.
If you are considering full-arch restoration, the most useful next step is not to look for the fastest promise. It is to get a clear diagnosis and a plan that explains what is possible in your anatomy, what trade-offs exist, and how the team intends to make the result predictable.
Comments (0)