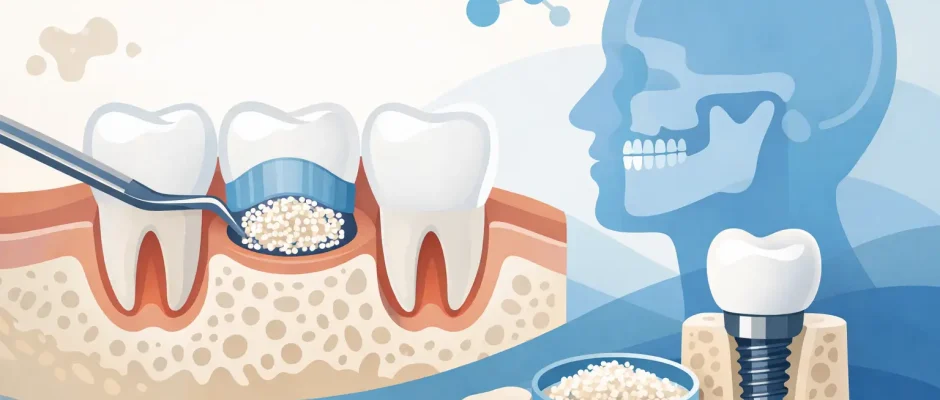
Why bone matters before an implant
A patient is often told, “You need more bone before we can place an implant,” and that sentence can sound bigger than it is. In practice, bone augmentation dentistry is a set of well-established surgical techniques used to rebuild areas of the jaw where bone volume is no longer enough for a stable, correctly positioned implant.
This matters because an implant does not simply fill an empty space. It must be anchored in bone with the right height, width, and density, and it should be placed in a position that supports both function and esthetics. If the bone is too thin or too low, the surgeon is forced into compromise – and compromise in implant surgery often shows up later as reduced stability, difficult hygiene, gum recession, or an unnatural crown position.
Why bone loss happens
Bone loss after a tooth is not an exception. It is the usual biological response. Once a tooth is removed, the jaw no longer receives the same functional load through the root, and the surrounding bone begins to shrink. The first changes can happen quickly, especially during the first months after extraction.
The pattern depends on the clinical situation. Long-standing missing teeth often lead to horizontal and vertical ridge resorption. Chronic infection around a failing tooth can destroy bone even before extraction. In the upper back jaw, the maxillary sinus may expand downward over time, leaving less available bone for implants. Gum disease, trauma, previous surgeries, and removable dentures can also contribute.
For that reason, bone deficiency is common even in otherwise healthy patients. It is not a sign that something unusual happened. It simply means the treatment plan needs to respect the anatomy that is present today, not the anatomy that was there years ago.
When bone augmentation dentistry is needed
Not every patient with bone loss needs grafting, and not every implant requires a separate augmentation procedure. The decision depends on three things: the amount of available bone, the planned implant position, and the long-term restorative goal.
If enough native bone is present to place an implant in a prosthetically correct position with good primary stability, augmentation may be unnecessary. In other cases, the implant can be placed at the same time as the graft. When bone is severely deficient, staged treatment is often safer and more predictable.
This is where careful diagnostics matter. A 3D scan does more than confirm that bone is missing. It shows the exact shape of the defect, the relation to neighboring teeth, nerves, and sinus anatomy, and whether simultaneous implant placement is realistic. In complex cases, digital planning and surgical guides help reduce guesswork and improve precision.
Common situations where augmentation is considered
The most typical indications include a narrow ridge after tooth loss, vertical deficiency that prevents adequate implant length or positioning, bone destruction from infection, and reduced bone height in the upper posterior jaw because of sinus pneumatization. Patients considering full-arch treatment may also need localized or broader augmentation depending on the anatomy and the planned protocol.
How bone is rebuilt
There is no single operation called “the bone graft.” Bone augmentation dentistry includes several techniques, and the right one depends on the defect.
Guided bone regeneration is one of the most common approaches. In simple terms, the surgeon places graft material into the deficient area and protects it with a membrane so the space can be maintained while the body forms new bone. This is frequently used for localized ridge defects around implant sites.
Socket preservation is a related concept performed at the time of extraction. Instead of allowing the socket to collapse as it heals, the site is grafted immediately to reduce future bone loss. This does not guarantee that no further augmentation will ever be needed, but it often makes later implant treatment easier and less invasive.
In the upper jaw, sinus floor elevation is used when the available bone under the sinus is limited. The sinus membrane is carefully elevated, and graft material is placed beneath it to create additional bone height. Depending on the residual bone, the implant may be placed at the same surgery or after healing.
For larger defects, block grafting or more advanced regenerative protocols may be considered. These cases require stricter planning, greater surgical precision, and realistic expectations about healing time.
What graft material is used
Patients often ask whether the new bone is “real bone” and where it comes from. The answer is that regeneration relies on a combination of the body’s healing capacity, the biology of the surgical site, and the material selected for that specific defect.
The graft may be autogenous, meaning taken from the patient’s own body, or it may be a biomaterial designed to support bone formation and remodeling. In many cases, the goal is not to create an exact copy of the original bone overnight. The goal is to build a stable, vascularized foundation that can support an implant over time.
Adjuncts such as PRF may also be used to support soft tissue healing and improve handling of the grafted area. These additions do not replace sound surgical technique, but when used appropriately, they can be valuable parts of a biologically respectful protocol.
Is it done at the same time as the implant?
Sometimes yes, sometimes no. This is one of the most important “it depends” decisions in implant surgery.
Simultaneous augmentation and implant placement can shorten treatment time and reduce the number of surgeries. It works best when enough native bone remains to stabilize the implant at the time of placement and when the defect can be predictably reconstructed around it.
A staged approach is usually better when primary stability would be weak, when the defect is extensive, or when infection and scarred tissue have made the site less favorable. Staging adds time, but in difficult anatomy it often improves safety and long-term predictability. Fast is attractive. Stable is better.
What recovery is really like
Most patients expect the recovery to be much harder than it actually is. In reality, healing after bone augmentation is usually manageable, especially when the procedure is planned carefully and soft tissues are handled gently.
Swelling for a few days is common. Mild bleeding or oozing on the first day can occur. Pressure, tenderness, and temporary limitations in chewing are expected. Pain is often less dramatic than patients fear, particularly when surgery is minimally traumatic and postoperative instructions are followed closely.
What matters most during recovery is protecting the grafted area. Excessive pressure from a denture, aggressive rinsing, smoking, poor oral hygiene, or returning too quickly to normal chewing can compromise healing. This is one reason a clear postoperative plan is not a small detail. It is part of the treatment itself.
Risks, limits, and realistic expectations
Bone augmentation has high value in modern implantology, but it is still surgery. Not every graft heals perfectly, and not every defect behaves the same way.
The main risks include infection, wound opening, partial graft loss, membrane exposure, delayed healing, and insufficient bone gain for the original plan. Smoking, uncontrolled diabetes, active periodontal disease, and poor oral hygiene can all reduce predictability. Thin soft tissues and large vertical defects are often more demanding than smaller contained defects.
This is why honest case selection matters. In some patients, the most sophisticated reconstruction is not automatically the best treatment. There are situations where a shorter implant, a different implant position, or an alternative prosthetic plan may be more reasonable than pursuing aggressive augmentation. Good surgery is not about doing the biggest procedure. It is about choosing the right one.
How to evaluate a treatment plan
If bone grafting has been recommended, ask a simple question: what problem is the augmentation solving? A strong answer should be specific. It may be needed to gain implant stability, improve prosthetic positioning, support the facial contour, or create enough bone height below the sinus.
You should also understand whether the plan is simultaneous or staged, what materials are being used, how healing will be monitored, and what the expected timeline looks like. When these details are explained clearly, anxiety usually drops. Patients handle surgery better when the path is visible.
In a practice focused on surgical dentistry and implantology, this planning is usually built around imaging, anatomy, soft-tissue conditions, and the final restoration – not just the question of whether an implant can physically fit somewhere in the bone. That distinction is especially important in demanding cases and is one reason many patients seek care from a surgeon who works with bone deficiency routinely, including complex implant cases in Tel Aviv.
Bone augmentation dentistry is not an obstacle
For many patients, hearing they need grafting feels like bad news. Clinically, it is often the step that makes a better result possible. Bone loss narrows the margin for error, but it does not automatically rule out implant treatment.
When augmentation is indicated, the real goal is not simply to add volume on a scan. It is to create the conditions for a stable implant, healthy surrounding tissue, and a restoration that feels reliable in daily life. The best plans are rarely the shortest ones. They are the ones that respect biology, reduce compromise, and give you a result worth keeping.
Comments (0)